Endometriosis Unveiled: A Patient's Tale for Medical Minds Part 1
- Isabella Mennillo: Academic Director

- Jan 28, 2024
- 4 min read
Updated: Feb 5, 2024

At the age of fourteen, endometriosis was first introduced into my vocabulary when one of my closest friends was diagnosed. I didn’t understand what endometriosis was, but I saw the pain that she dealt with every day, the medication she carried in her blazer pocket ‘just in case’ and the frequent doctor visits where they could not find an answer for her symptoms. In more recent years, my social media has been filled with other women who I grew up alongside sharing their diagnosis of endometriosis after searching for answers to their symptoms for years.
When introduced to women’s health in my second year of medical school, I sought answers as to what causes endometriosis and how it can be treated. This curiosity was met with a large number of unknowns. With more than 830,000 (14%) of Australian girls, women and those assigned female at birth experiencing endometriosis at some point in their lives, I couldn’t understand how we didn’t have answers to these questions. I want to change this.
I reached out to my two closest friends and asked them if they would be willing to share their journey with endometriosis. As a future healthcare professional, understanding the complexities of endometriosis is not merely a clinical exercise, but an exploration into the human side of medicine. This two-part blog post aims to bridge the gap between basic medical knowledge of this condition and empathetic care, offering insights that extend beyond our textbooks and lectures.
Clinical background:
Endometriosis is characterised by the growth of endometrial tissue (the tissue that normally lines the inside of the uterus), grows outside the uterus.
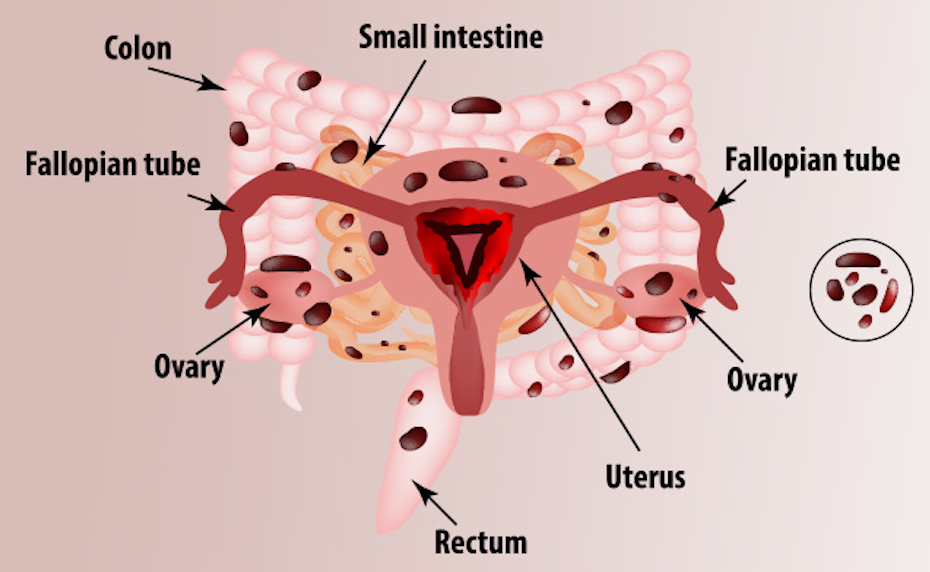
Common locations of endometriosis are:
· The ovaries
· Rectouterine pouch
· Fallopian tubes
· Bladder
· Cervix
· Peritoneum
· Extra-pelvic organs e.g. lung or diaphragm
Similar to the lining inside the uterus, endometriosis tissue reacts to the hormonal cycle in the same way as the endometrium does – it thickens in response to oestrogen, breaks down and bleeds with each menstrual cycle. However, this tissue is growing where it shouldn’t, and it cannot leave the body which can result in increased production of inflammatory mediators, pelvic adhesions and nerve dysfunction. The exact cause of endometriosis has not yet been determined, and often, the only way for individuals to be diagnosed is via laparoscopic surgery to biopsy the tissue.
Ok, now that we have briefly covered the clinical side of things, let's jump straight into it.
Endometriosis has a variable set of symptoms, which often contributes to a 6.5-year delay in diagnosis. I asked C if she could detail some of her symptoms and her journey to diagnosis to help us get a better understanding of how endometriosis presents.
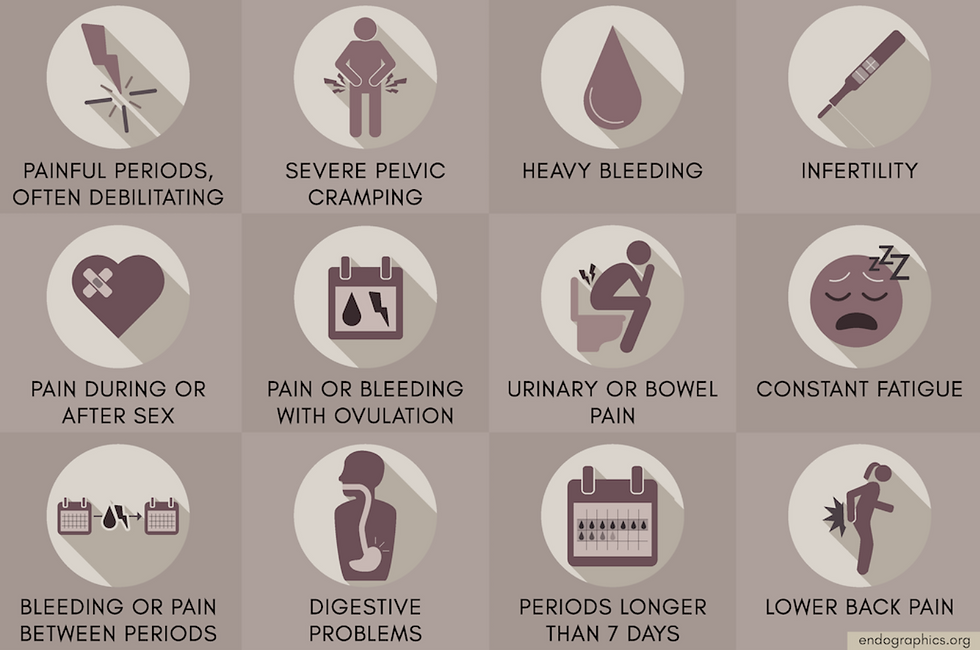
Symptoms:
- Debilitating cramping around the stomach, lower back and pelvis
- Fatigue
- Nausea
- Not feeling like her usual self
- Unable to participate in daily activities
The journey to diagnosis:
C received her diagnosis at the age of fourteen, four months after seeking medical attention.
‘When I first attended a GP to tell them about my symptoms they were passed off as stomach pains or potential issues with my bowel. When communicating my symptoms and needs to healthcare providers I was concerned that how I was explaining it wouldn’t come across right. Was I explaining it to the level it felt? Would they dismiss me about how bad it is? I was then referred to a paediatric gastroenterologist for further investigations, which showed nothing.’- C
C later attended the Emergency Department with worsening symptoms. This led to the discovery of her endometriosis when undergoing a laparoscopic surgery to remove a painful ovarian cyst. Her surgeon found abnormal tissue, which was then sent to pathology, and later diagnosed as endometriosis.
Clinical point: When endometriosis involves the ovaries, cysts called endometriomas may form. The surrounding tissue can become irritated and form scar tissue. Bands of fibrous tissue called adhesions may also form which can result in pelvic organs and tissues to adhere to each other.
As C was only fourteen, she was concerned if the symptoms she was experiencing were ‘normal’.
‘At that time, schools and the media didn’t educate young women surrounding what to expect regarding your menstruation and when to seek medical help. I also didn’t have a lot of people that I could relate to about what I was experiencing and that made me feel quite isolated.’- C
After her initial diagnosis, C was referred to a gynaecologist.
The role of her gynaecologist included:
- Discussing the potential treatment options relevant to C’s age
- How to best manage C’s symptoms long-term
C still sees the same gynaecologist for the ongoing management of her symptoms five years post diagnosis.
C mentioned that her diagnosis of endometriosis raised other personal questions and concerns. When empowered to research her condition further, she came across statistics that tied endometriosis to infertility.
‘Ageing as a woman with endometriosis still brings about concerns regarding my fertility. It is known that around 30-50% of women with endometriosis can experience issues with their fertility. As someone who definitely wants to be a mother one day, naturally I am concerned how my condition will impact this goal. Due to this, education and communicating with dedicated healthcare professionals’ overtime is so crucial.’ - C
The link between endometriosis and infertility underscores the need for ongoing communication with healthcare professionals and the significance of education for individuals with the condition. As future healthcare professionals, C's story prompts us to recognise the significance of not only addressing the physical aspects of the condition but also the emotional and social dimensions that contribute to the overall well-being of individuals affected by endometriosis. In our pursuit of empathetic care, understanding the human side of medicine involves acknowledging and addressing the multifaceted aspects of living with conditions like endometriosis. By sharing stories, fostering awareness, and promoting open dialogue, we can contribute to a more supportive and informed healthcare environment for those affected by endometriosis and similar conditions.
Stay tuned for Part 2 of this series where we discuss the management of Endometriosis....

Comments